Tuberculosis is a contagious bacterial infection caused by Mycobacterium tuberculosis. It most often affects the lungs (pulmonary TB), but it can also affect other parts of the body (extrapulmonary TB). Normally, when someone with active TB coughs or sneezes, tiny droplet nuclei containing bacteria are released and can be inhaled by another person, leading to infection. If the body cannot control the bacteria, they multiply and cause disease.
Reasons Behind Tuberculosis and Its Risk Factors
Several factors increase the risk of developing TB:
- Infection with Mycobacterium tuberculosis: Exposure to someone with active pulmonary TB is the primary cause.
- Weakened immune system: Conditions like HIV, diabetes, malnutrition, or immunosuppressive therapy reduce the body’s ability to control the bacteria.
- Poor living conditions, including overcrowding, inadequate ventilation, air pollution, and poverty, increase the risk.
- Lifestyle & comorbidities: Smoking, alcohol abuse, and diseases like diabetes make TB more likely.
- Latent infection: Many people carry latent TB, which can become active when immunity falls.
How Tuberculosis Impacts Different Organs and Systems
While the lungs are most commonly involved, TB can affect multiple organs and systems:
- Lungs (Pulmonary TB): The most common symptoms include cough, chest pain, and hemoptysis (coughing up blood).
- Lymph nodes (especially neck): Enlarged nodes are often seen in extrapulmonary TB.
- Bones and joints: TB can cause skeletal TB (e.g., spine Pott’s disease).
- Kidneys and urinary tract: TB may affect these, causing urinary symptoms.
- Brain and meninges: TB meningitis is a serious form.
- Gastrointestinal tract: TB may infect the intestines.
- Other organs include the skin, pericardium (the heart’s covering), and others. Because TB can spread via blood or lymph, and because immunity is central, many parts of the body may be involved when the infection is not confined to the lungs.
Types of Tuberculosis
There are several classifications of TB:
- Active TB disease: The bacteria are active, symptoms are present, and the person may be infectious.
- Latent TB infection (LTBI): The person is infected with the bacteria but shows no symptoms and is not infectious. The bacteria remain dormant and can activate later.
- Pulmonary TB: TB located in the lung tissue.
- Extrapulmonary TB: TB located in organs other than the lungs (lymph nodes, brain, bones, kidneys, etc.).
- Multidrug-resistant TB (MDR-TB) / Extensively drug-resistant TB (XDR-TB): TB strains resistant to first-line (and second-line) TB drugs requiring specialized therapies.
- Each type has different implications for treatment duration, follow-up, and public health precautions.
India’s Present Health Data and Statistical Trends
- India has the highest burden of TB globally, contributing approximately 26-28% of global incident TB cases.
- In 2022, the estimated incidence in India was about 2.77-2.82 million new TB cases (~195-199 cases per 100,000 population).
- In India, about one-third of the adult population (>15 years) may carry latent TB infection (TBI), about 31% according to a 2019-21 survey.
- The incidence and mortality of TB in India have fallen since 2015 incidence down by about 17-18%, and deaths similarly reduced with intensified efforts.
- TB disproportionately affects vulnerable socio-economic groups and is strongly linked with co-morbidities like diabetes and HIV.
How Can Tuberculosis Be Treated and Managed?
TB treatment and control require early detection, appropriate therapy, and public health measures:
- Diagnosis: Includes sputum microscopy, GeneXpert/CBNAAT, chest X-ray, culture & drug susceptibility testing for resistant cases.
- Drug therapy: For drug-sensitive TB, standard 6-month regimen (4 drugs for 2 months, then 2 drugs for 4 months) under directly observed treatment (DOT). For drug-resistant TB, longer and more complex therapy is required.
- Latent TB therapy: Preventive treatment for those with latent TB at high risk of activation.
- Supportive care: Nutritional support, monitoring and managing co-morbidities (e.g., diabetes), and regular follow-up.
- Public health measures: Isolation when infectious, contact tracing, screening in high-risk populations, improving living conditions, vaccination (BCG) where applicable.
Precautions & Preventive Measures
- Ensure good ventilation and reduce overcrowding at home and workplaces.
- Cover mouth when coughing or sneezing; use masks in high-risk settings.
- Avoid prolonged close contact with a person known to have active TB until they are treated.
- Screen high-risk people (contacts of TB patients, people with HIV, diabetes, malnutrition).
- Maintain good nutrition, healthy weight, and manage co-morbidities (such as diabetes, HIV).
- Avoiding smoking and reducing alcohol abuse both increase TB risk.
- Adhere strictly to treatment if diagnosed; incomplete treatment fosters drug resistance.
- Participate in vaccination programs (BCG for children, other interventions as per local guidelines).
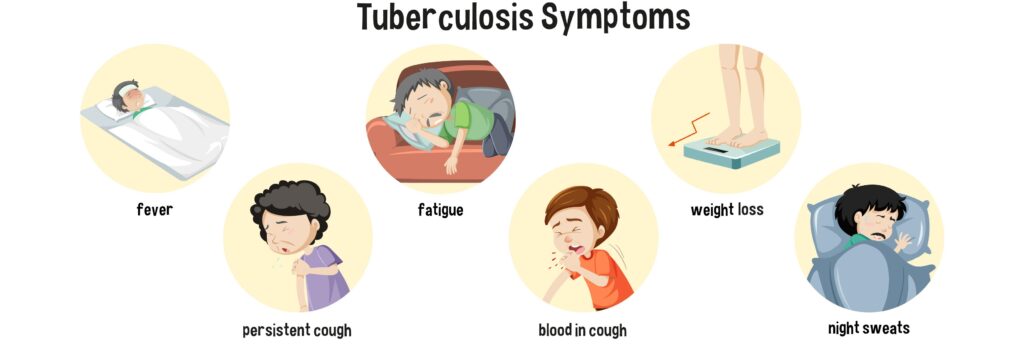
- Raise awareness: recognise symptoms like persistent cough, fever, night sweats, weight loss; seek medical evaluation early.


Leave a Reply